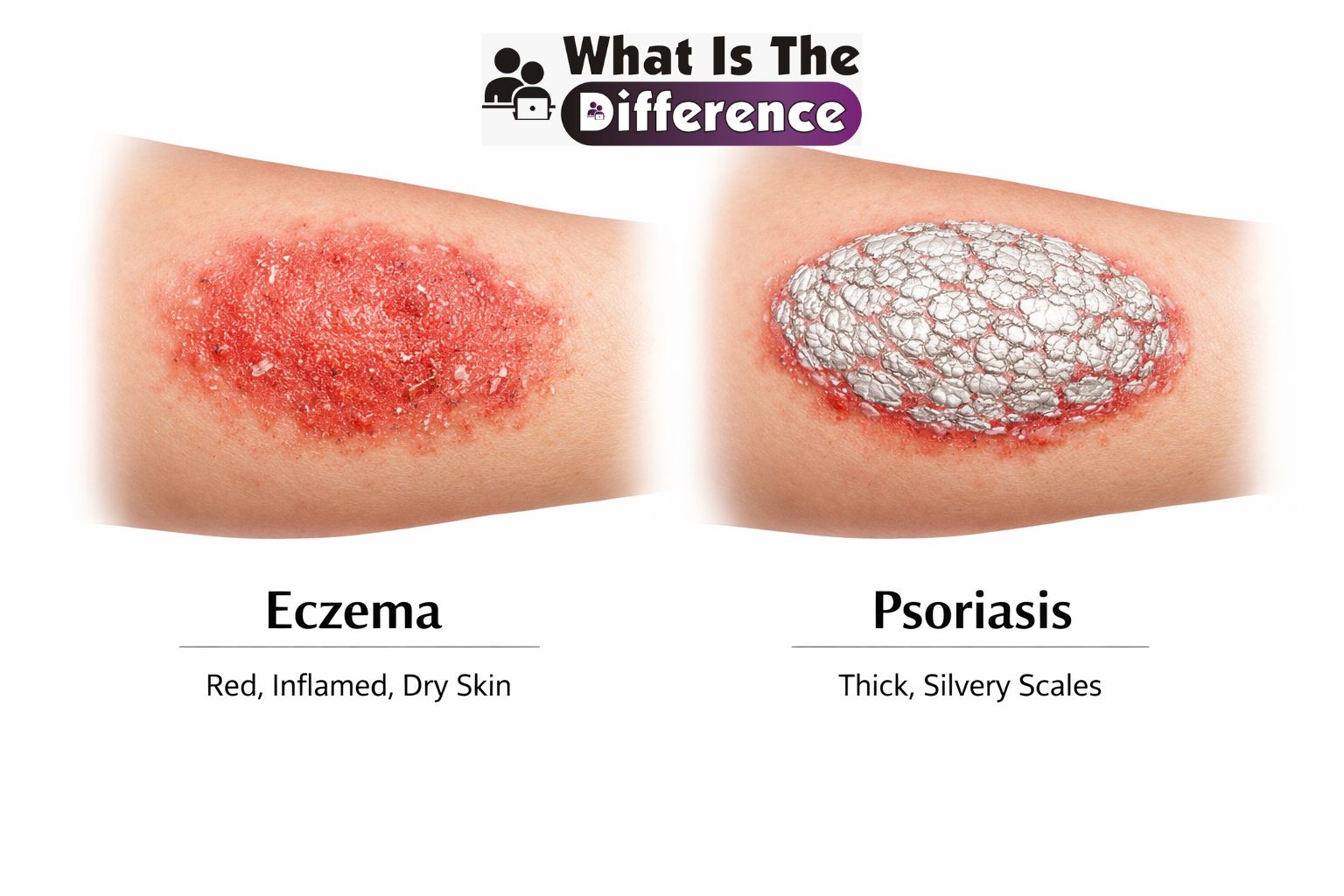
Skin conditions that cause redness, itching, and irritation can often look very similar at first glance. Two of the most commonly confused conditions are eczema and psoriasis. Both can create patches of inflamed skin, dryness, and discomfort, which is why many people struggle to tell them apart.
Understanding what is difference between eczema and psoriasis is important because each condition has its own causes, triggers, and treatments. While they share some symptoms, they are medically distinct diseases that require different approaches to care.
Dermatologists often explain that eczema is usually linked to skin sensitivity and environmental triggers, whereas psoriasis is an autoimmune disorder involving the body’s immune system.
This article explores the signs, causes, and key facts about both conditions so readers can better understand how they differ and how they are managed.
BIO
| Feature | Eczema | Psoriasis |
|---|---|---|
| Medical Nature | Inflammatory skin condition often linked to allergies | Autoimmune disease affecting skin cell growth |
| Main Cause | Weak skin barrier and environmental triggers | Immune system speeds up skin cell production |
| Skin Appearance | Red, dry, irritated patches | Thick red plaques with silvery scales |
| Texture | Rough and dry skin | Thick, raised, and scaly skin |
| Itching Level | Usually very itchy | Mild to moderate itching, sometimes burning |
| Common Body Areas | Inside elbows, behind knees, face, neck | Elbows, knees, scalp, lower back |
| Age of Onset | Often begins in childhood | Commonly appears in adults |
| Skin Thickness | Skin may become thick from scratching | Plaques naturally thick due to rapid cell growth |
| Triggers | Allergens, soaps, weather, stress | Stress, infections, medications, cold weather |
| Contagious | Not contagious | Not contagious |
| Typical Treatment | Moisturizers, steroid creams, avoiding triggers | Topical treatments, phototherapy, systemic medication |
| Healing Pattern | Flare-ups linked to irritants or allergies | Chronic condition with immune-related flare-ups |
Understanding Eczema
What Is Eczema?
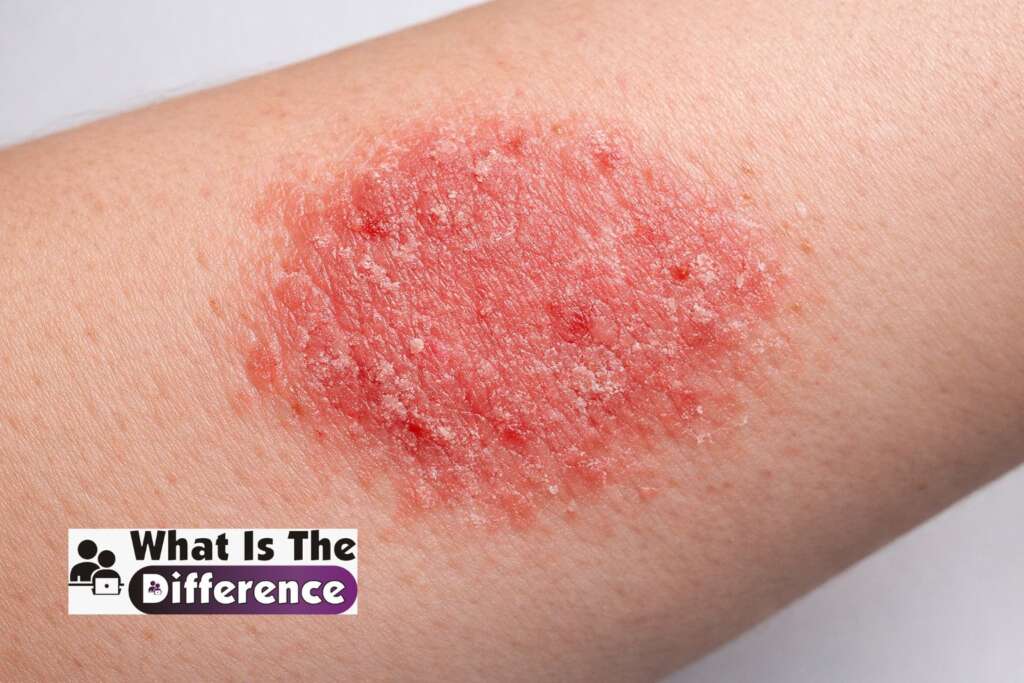
Eczema is a common inflammatory skin condition that causes dry, itchy, and irritated skin. The most common type is atopic dermatitis, which often begins in childhood but may continue into adulthood.
In eczema, the skin’s protective barrier becomes weakened, allowing irritants and allergens to affect the skin more easily. As a result, the immune system reacts and creates inflammation, redness, and intense itching.
Although eczema can appear anywhere on the body, it is especially common on the face, hands, neck, and in skin folds such as behind the knees or inside the elbows.
Eczema is not contagious, but it can be chronic, meaning it may flare up from time to time depending on triggers.
Common Symptoms of Eczema
The symptoms of eczema can vary from mild irritation to severe inflammation. However, several signs are commonly associated with the condition.
People with eczema often experience extremely itchy skin. In many cases, itching is the most intense symptom and may even disrupt sleep. Scratching the affected areas can worsen the inflammation and sometimes cause skin damage.
Other symptoms include dry or rough skin patches that may appear red, dark, or inflamed depending on the person’s skin tone. The skin can sometimes crack or ooze fluid, especially during severe flare-ups.
With repeated irritation and scratching, the skin may become thicker and leathery over time. These symptoms often appear in cycles, with flare-ups followed by periods of improvement.
What Causes Eczema
Eczema usually develops because of a combination of genetic and environmental factors. People with eczema often have an immune system that reacts strongly to certain substances.
Common triggers include irritants such as soaps, detergents, fragrances, and cleaning chemicals. Allergens like dust, pollen, pet dander, or certain foods may also cause flare-ups. Cold weather, dry air, and stress are additional factors that can worsen symptoms.
Many individuals with eczema also have other allergic conditions such as asthma or hay fever, which suggests that the immune system plays a role in the disease.
Types of Eczema
Eczema is not a single disease but a group of related conditions. Dermatologists recognize several types, including:
Atopic dermatitis, the most common form, usually begins in childhood and causes persistent itchy rashes.
Contact dermatitis, which occurs when the skin reacts to irritants or allergens such as cosmetics, chemicals, or certain metals.
Dyshidrotic eczema, which produces small blisters on the hands and feet.
Nummular eczema, which creates round or coin-shaped patches on the skin.
Seborrheic dermatitis, a form that commonly affects the scalp and areas rich in oil glands.
Each type may have different triggers, but they all involve inflammation and irritation of the skin.
Understanding Psoriasis
What Is Psoriasis
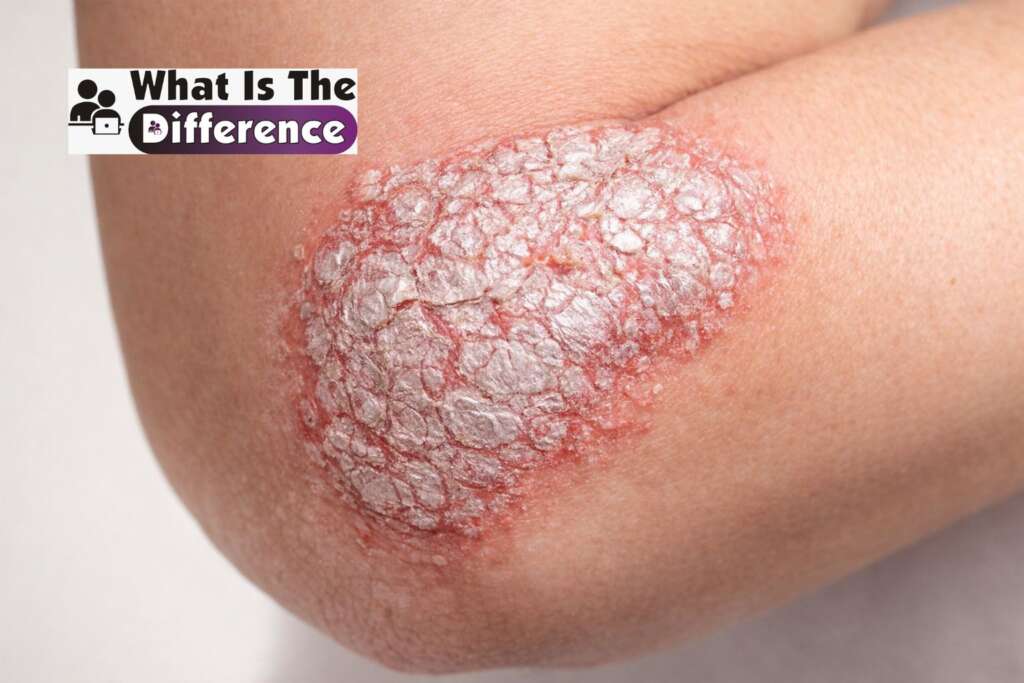
Psoriasis is a chronic autoimmune disease that affects the skin. Unlike eczema, psoriasis occurs when the immune system mistakenly attacks healthy skin cells. This reaction speeds up the skin’s life cycle and causes new cells to grow too quickly.
Normally, skin cells take several weeks to grow and shed. In psoriasis, the process may take only a few days. Because of this rapid growth, skin cells accumulate on the surface and form thick, scaly patches known as plaques.
Psoriasis is also a long-term condition with periods of flare-ups and remission.
Common Symptoms of Psoriasis
Psoriasis produces distinctive skin changes that often look different from eczema once examined closely.
One of the most recognizable symptoms is the presence of thick red patches of skin covered with silvery or white scales. These plaques may appear on different parts of the body, including the scalp, elbows, knees, and lower back.
Some people experience itching, but psoriasis is more commonly associated with burning, soreness, or stinging sensations.
In more severe cases, psoriasis may also affect the nails, causing pitting or discoloration. Some individuals develop joint inflammation known as psoriatic arthritis.
What Causes Psoriasis
The exact cause of psoriasis is not fully understood, but researchers know that it is strongly related to immune system activity.
In psoriasis, certain immune cells become overactive and release signals that speed up skin cell production. As these cells multiply rapidly, they accumulate on the skin’s surface and create plaques.
Genetics also plays an important role. Many people with psoriasis have family members who also have the condition.
Common triggers that may cause flare-ups include infections, stress, skin injuries, certain medications, and cold weather.
Types of Psoriasis
Like eczema, psoriasis appears in several forms.
The most common type is plaque psoriasis, which accounts for the majority of cases and produces thick scaly patches.
Guttate psoriasis appears as small drop-shaped spots, often triggered by infections.
Inverse psoriasis develops in skin folds such as under the arms or breasts.
Pustular psoriasis causes pus-filled blisters surrounded by red skin.
Erythrodermic psoriasis is a rare but severe form that causes widespread redness and peeling of the skin.
Each type may require different treatment approaches.
What Is Difference Between Eczema and Psoriasis
Difference in Appearance
One of the easiest ways to understand what is difference between eczema and psoriasis is by examining how the skin looks.
Eczema typically produces dry, inflamed patches that may appear rough or scaly but are usually not thick. The edges of eczema patches may be less clearly defined.
Psoriasis, on the other hand, often forms thick plaques with distinct borders and noticeable silvery scales. These plaques may feel raised compared to the surrounding skin.
Because of these visible differences, dermatologists can often identify the condition through a physical examination.
Difference in Causes
Another major difference lies in the underlying cause of each condition.
Eczema is commonly associated with a weakened skin barrier and sensitivity to environmental triggers such as allergens or irritants.
Psoriasis is an autoimmune disease in which the immune system causes rapid growth of skin cells.
This difference is important because it affects the way doctors approach treatment.
Difference in Itching and Discomfort
The sensation experienced by patients can also vary between the two conditions.
Eczema is usually extremely itchy, and scratching may lead to skin damage or infection. Many patients describe the itching as intense and difficult to control.
Psoriasis may itch as well, but the sensation is often described as burning or stinging rather than constant itching.
These differences in sensation can sometimes help doctors distinguish between the conditions.
Difference in Affected Body Areas
Another key factor is the location where symptoms appear.
Eczema commonly affects areas where the skin bends, such as inside the elbows, behind the knees, and on the neck. It can also appear on the hands and face.
Psoriasis tends to appear on the outer surfaces of joints such as the elbows and knees, as well as the scalp and lower back.
While both conditions can appear anywhere on the body, these typical patterns often provide important clues.
Difference in Age of Onset
Age of onset also helps explain what is difference between eczema and psoriasis.
Eczema often begins in infancy or childhood. Many children experience symptoms early in life, although some eventually outgrow the condition.
Psoriasis is more likely to develop later, often appearing in adolescence or adulthood.
However, both conditions can occur at any age.
Similarities Between Eczema and Psoriasis
Although they are different diseases, eczema and psoriasis share several similarities.
Both are chronic inflammatory skin conditions that cause redness, irritation, and dry skin.
They can both appear in cycles with flare-ups followed by periods of improvement.
Both conditions may also worsen due to stress, infections, or environmental factors.
In addition, eczema and psoriasis may require ongoing treatment and careful skin care to control symptoms.
Because the symptoms can overlap, many people mistakenly believe they have one condition when they actually have the other.
Diagnosis and Medical Evaluation
How Doctors Diagnose Eczema
Doctors usually diagnose eczema through a physical examination of the skin and a review of the patient’s medical history.
In some cases, allergy testing may be recommended to identify triggers. Doctors may also ask questions about family history and environmental factors.
How Psoriasis Is Diagnosed
Psoriasis is also typically diagnosed through a physical examination. The appearance of the plaques and their location on the body often provide strong clues.
In rare cases, a dermatologist may perform a skin biopsy to confirm the diagnosis.
Treatment Options for Eczema
Treatment for eczema focuses on controlling symptoms and preventing flare-ups.
Moisturizers are often the first line of treatment because they help repair the skin barrier and reduce dryness.
Doctors may also prescribe topical corticosteroids or anti-inflammatory creams to reduce redness and itching.
Antihistamines may be used to help control itching, especially at night.
Lifestyle changes such as avoiding irritants, using gentle skin care products, and managing stress can also help prevent flare-ups.
Treatment Options for Psoriasis
Psoriasis treatment depends on the severity of the condition.
Mild cases may be treated with topical creams that reduce inflammation and slow skin cell growth.
Phototherapy, which involves controlled exposure to ultraviolet light, can help moderate symptoms in some patients.
Moderate to severe psoriasis may require systemic medications or biologic therapies that target the immune system.
These treatments aim to control the immune response that causes the rapid growth of skin cells.
When to See a Doctor
Although many people attempt to manage skin conditions at home, it is important to seek medical advice if symptoms persist.
A doctor should be consulted if skin irritation becomes severe, spreads rapidly, or causes significant pain.
Professional diagnosis is also essential because eczema and psoriasis require different treatment strategies.
Tips for Managing Skin Health
Maintaining healthy skin can help reduce flare-ups of both eczema and psoriasis.
Regular moisturizing is one of the most effective strategies for preventing dryness and irritation.
Using mild soaps and avoiding harsh chemicals can protect the skin’s natural barrier.
Stress management, balanced nutrition, and proper hydration may also support overall skin health.
Although these habits cannot cure either condition, they can help reduce the frequency and severity of symptoms.
Conclusion
Understanding what is difference between eczema and psoriasis is essential for recognizing symptoms and seeking appropriate care.
Eczema is primarily related to skin sensitivity and environmental triggers, while psoriasis is an autoimmune condition that causes rapid skin cell growth. These underlying differences lead to variations in appearance, itching, location, and treatment methods.
Although both conditions can be uncomfortable and persistent, modern medical treatments can effectively manage symptoms and improve quality of life.
Anyone experiencing ongoing skin irritation should consult a healthcare professional for accurate diagnosis and personalized treatment. Early care and proper management can make a significant difference in controlling both eczema and psoriasis.
What Is the Difference Between DO and MD in the U.S. Healthcare System?
FAQs
1. What is the main difference between eczema and psoriasis?
The main difference is the underlying cause. Eczema is usually related to skin sensitivity, allergies, and environmental triggers that weaken the skin barrier. Psoriasis, however, is an autoimmune condition where the immune system speeds up skin cell growth, leading to thick scaly patches.
2. Which condition causes more itching, eczema or psoriasis?
Eczema typically causes more intense itching than psoriasis. Many people with eczema experience constant itching that can become worse at night. Psoriasis may also itch, but it often causes a burning or stinging sensation instead.
3. Can eczema turn into psoriasis?
No, eczema cannot turn into psoriasis. They are separate medical conditions with different causes. However, because their symptoms may look similar, people sometimes confuse one condition for the other without a proper medical diagnosis.
4. Where do eczema and psoriasis usually appear on the body?
Eczema commonly appears in skin folds such as inside the elbows, behind the knees, and around the neck or face. Psoriasis usually appears on the scalp, elbows, knees, and lower back where thick plaques can develop.
5. Is there a cure for eczema or psoriasis?
Currently, there is no permanent cure for either eczema or psoriasis. However, both conditions can be managed with proper treatment, skincare routines, and avoiding triggers that cause flare-ups.